Creating Equity in COVID-19 Testing and Vaccine Distribution
June 7, 2021541 views0 comments
As chief of the Division of General Obstetrics and Gynecology for Penn Medicine, Dr. Florencia Greer Polite has spent many satisfying work days delivering babies and taking care of her female patients. But it was something out of her regular routine that recently became a defining moment in her career.
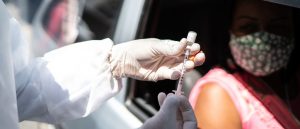 When the COVID-19 vaccine rollout began at the Hospital of the University of Pennsylvania, Polite was worried about the lack of compliance, especially among minority staffers. As a Black woman, she understood vaccine hesitancy; as a physician, she felt compelled to do something about it.
When the COVID-19 vaccine rollout began at the Hospital of the University of Pennsylvania, Polite was worried about the lack of compliance, especially among minority staffers. As a Black woman, she understood vaccine hesitancy; as a physician, she felt compelled to do something about it.
“What was literally keeping me up at night were these issues of hesitancy,” Polite said. “I made the personal decision to get vaccinated on the first day at Penn Medicine, despite my own personal hesitancy. I’m not an early adopter of anything, but I felt like this was an opportunity for me to get vaccinated, to be public about what that experience was like, and to hopefully educate my family, my friends, and my community and my patients.”
Polite took her advocacy a step further, helping to create Operation CAVEAT at the hospital — an acronym that stands for Covid Acceptance Vaccine Education and Adoption Taskforce. She spoke recently to Wharton management professors Stephanie Creary and Aline Gatignon about the initiative and the broader issue of equity in COVID-19 testing and vaccine distribution. David Casey, chief diversity officer and senior vice president of workforce strategies at CVS Health, also joined the conversation, which was part of Creary’s Leading Diversity@Work podcast series. (Listen to the podcast above.)
Part of Casey’s job includes figuring out how his company can reach minority populations to help them get access to health care, including COVID-19 testing and vaccines. Since the pandemic began in early 2020, numerous studies have documented the disproportionate toll that it is taking on Black, Hispanic and Native American communities.
“We’ve all heard the saying that your ZIP code matters more than your genetic code when it comes to health care,” Casey said. “You can literally go less than a mile, and the health care experiences of the individuals in that part of the community can be vastly different than they are just a mile down the road.”
Polite agreed, noting that health care disparities are about racism — not race. “There’s nothing inherently different about a Black or Latinx patient that makes them more likely to die of COVID, but there are a number of systemic factors that affect that mortality or that death rate,” she said.
‘A Three-headed Beast’
Polite said she thinks about COVID-19 as “a three-headed beast” for communities of color. First, there is the increased mortality of minority populations due to COVID-19. Many working-class Black and Hispanic people have jobs with high exposure to the public and no personal protective equipment, and they may live in multigenerational homes — all factors that increase the risk of contracting and dying from the disease.
The second head is vaccine access. Broadly, that’s about how states are getting the doses to cities, towns, villages, and hamlets. More specifically, how are authorities and health care leaders making sure that the most vulnerable people get the injections with as few barriers as possible?
The third head of the beast is vaccine hesitancy, which Polite pinpointed as a problem stemming from America’s legacy of systemic racism and inequality.
“We got [to this point] over 400 years. We’re not going to turn around in two weeks or a month,” she said. “It’s going to take a lot of very intentional small steps over a long time. But we have many, many, many people to bring along who, quite frankly, are often in leadership positions, which might make this a more challenging burden to overcome.”
Through Operation CAVEAT, Polite and her colleagues tackled these issues in three steps:
Black physicians who were vaccinated created a one-page information sheet that was distributed to departments with the highest number of minority employees, including environmental services, dietary services, patient transport and materials management. The sheet outlined the reasons why the doctors were vaccinated and encouraged the employees to do the same. It was an important step, Polite said, because most of Penn’s information was being disseminated by email, and many of those employees are outsourced and thus, do not have access to Penn email.
The team worked with the public relations department to develop informational screen savers that were displayed across the hospital, especially in break rooms where the targeted employees clock in and out. The screen savers specifically addressed myths about the vaccine by providing the facts, Polite said.
The targeted employee groups commonly hold “huddles” with their supervisors across shifts. Black and non-Black physicians attended the huddles to answer any questions about the vaccines. These meetings were unscripted and informal, giving employees a chance to voice their concerns and talk comfortably.
These steps, along with others designed to give employees easy, on-site access to the vaccines, helped the hospital make a measurable improvement in vaccine compliance, Polite said.
‘Trusted Faces and Trusted Places’
The hospital’s experience in reaching minority employees was a microcosm of the work Casey does to reach out to minority communities across the U.S. Even with 10,000 stores, Casey said that CVS Health knew it couldn’t get the job done alone. That’s why the company has continuing partnerships with nonprofits, community centers, free and charitable clinics, faith-based organizations, civic leaders — just about anyone that can help spread the health care message to those who need it most.
Borrowing a phrase he heard from local partners, Casey said that to deliver vaccines effectively into Black and brown communities, “You have to have trusted faces and trusted places.”
“Where are the places people typically go, that they’re used to going, that they may still be going to during COVID?” he said. “Is it a community free clinic? Is it their church? Is it the grocery store? Where is it that people are going, and how can we offer vaccines there, as opposed to our store? We wanted to take health care to the community, not just where people live, but how they live.”
Casey and Polite urged others who are in leadership positions to find and evaluate the racial disparities within their organizations, create a collaborative plan with realistic solutions, deploy the plan, then measure the outcomes. Recognize the difference between equity and equality, and never stop talking about it — even when it makes people uncomfortable.
Casey recalled posting some numbers on his LinkedIn page early in the pandemic that documented the disproportionately high death rate among Blacks and Hispanics. He immediately got push-back from a few people who criticized him for talking about race. Yet no one challenged the conversation when data showed how the disease was ravaging the elderly.
“As soon as we saw data…on the Black and African American community, then part of the narrative became, ‘Well, why are we talking about race?’ Where did that hesitation come from? Where did that push-back come from?” Casey said. “Making sure that equity is being thought about at the outset, not as an afterthought, is a challenge. It was a challenge for us in the beginning, and it’s a challenge for all of us involved in health care to think about going forward.”
‘Food for My Soul’
Through the Mercy/Penn Medicine & The Community Vaccine Collaborative, Polite volunteered to administer COVID-19 vaccines. She remembers vaccinating 80 people in one day, and 70 of them were Black. The experience was gratifying in ways she did not expect, even for a doctor used to helping people. Hesitancy and advocacy work is exhausting, she said, but this was “icing on the cake.”
“At the end of the day, it was like food for my soul,” she said. “It was one of the best days. I came home, and my kids were like, ‘You were super tired when you went, and you look way less tired now.’”
